Acetaminophen Overdose Risk Calculator
Check Your Acetaminophen Risk
This calculator estimates your overdose risk based on the article's critical guidelines. Remember: Every hour without treatment reduces antidote effectiveness by 10%.
Every year, thousands of people in the UK and across the world suffer liver damage from medications they took without knowing the risk. It’s not just about overdosing on painkillers. Sometimes, it’s the antibiotic you took for a sinus infection, the turmeric capsule you started for joint pain, or even the statin your doctor prescribed for cholesterol. This isn’t rare. It’s called drug-induced liver injury (DILI), and it’s one of the most under-recognized dangers in modern medicine.
What Exactly Is Medication-Related Liver Damage?
DILI happens when a drug - prescription, over-the-counter, or herbal - harms your liver. Your liver is your body’s main detox center. It breaks down almost everything you take. But sometimes, that process goes wrong. Instead of safely processing the drug, your liver cells get damaged. This can happen even at normal doses. You don’t need to take too much. You just need to be sensitive to it.
Antibiotics like amoxicillin-clavulanate are the top offenders, making up over 16% of cases. Anticonvulsants, NSAIDs like ibuprofen, and herbal supplements like green tea extract are close behind. In the UK, supplements cause about 1 in 5 cases of liver injury. And here’s the scary part: 70% of severe cases could be avoided if people knew the signs and acted fast.
The Hidden Signs - Don’t Wait for Jaundice
Most people think liver damage means yellow skin or eyes. That’s jaundice. But by the time you turn yellow, your liver is already badly hurt. The real warning signs come earlier - and they’re easy to ignore.
- Unexplained fatigue that doesn’t get better with rest
- Dark urine - like tea or cola
- Itchy skin without rash or dryness
- Loss of appetite or nausea that lasts more than a few days
- Pain under your right ribs - not just bloating
- Light-colored stools - pale, clay-colored poop
One patient in Manchester told her GP she felt tired and itchy after starting amoxicillin for a chest infection. She was told it was “just allergies.” Two weeks later, her urine turned dark. Her liver enzymes were 15 times higher than normal. She needed hospital care.
These symptoms often appear 1 to 8 weeks after starting a new medication. For antibiotics, it’s usually around day 15. For herbal supplements? It can be as short as a week or as long as a year. That’s why people miss the link.
When to Go to the Emergency Room - Not Your GP
Not every odd feeling means liver damage. But if you’ve started a new medication in the last 8 weeks and you have jaundice plus any two of these, you need to go to A&E right away:
- Dark urine
- Pain in the upper right side of your belly
- Nausea or vomiting that won’t go away
This isn’t a “wait and see” situation. The longer you wait, the more damage you risk. In severe cases, your liver can shut down in days. That’s called acute liver failure. And it’s deadly without fast treatment.
For acetaminophen (paracetamol) overdose, timing is everything. If you take too much - even just 8 pills at once - you have less than 8 hours to get N-acetylcysteine, the antidote. Every hour you wait cuts the treatment’s effectiveness by 10%. The maximum safe daily dose for healthy adults is 3,000 mg. For anyone with liver disease or who drinks alcohol, it’s 2,000 mg. Many cold and flu meds contain acetaminophen. Read the labels.
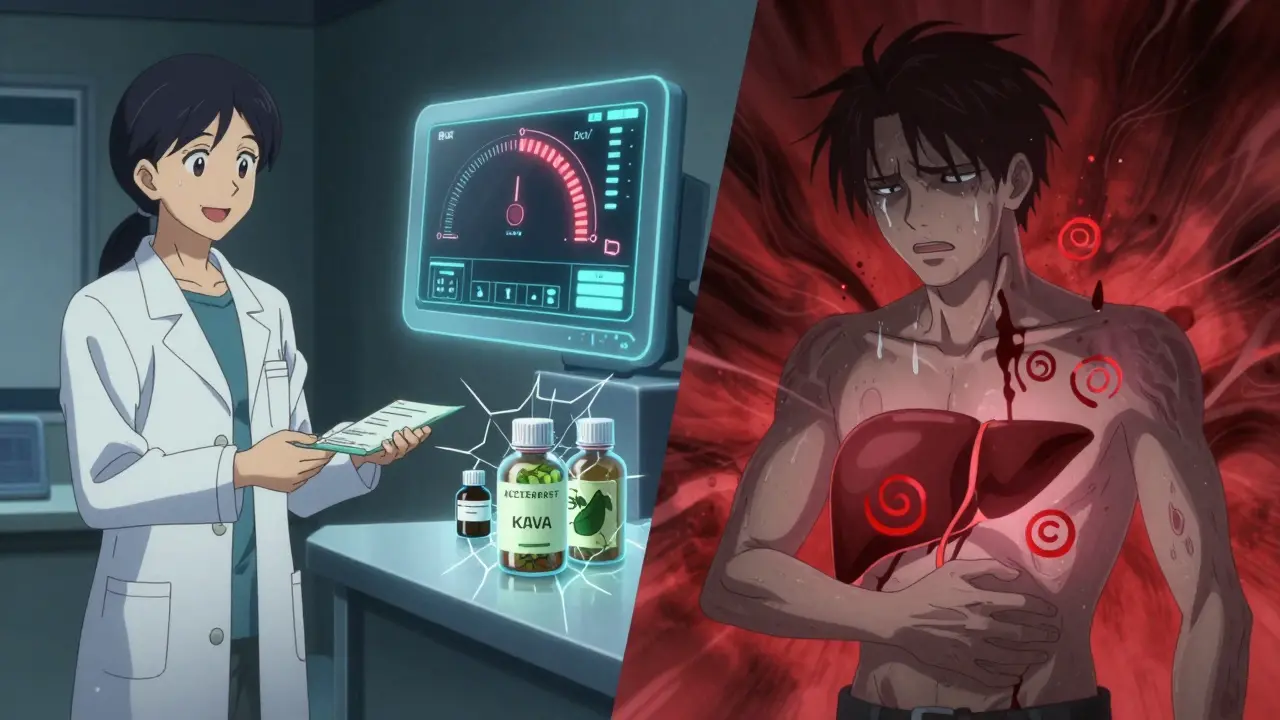
Supplements Are Not Safe Just Because They’re Natural
“It’s just turmeric,” people say. “It’s good for inflammation.” But green tea extract, kava, and even high-dose vitamin A have caused liver failure. In the UK, green tea extract alone is linked to 37% of supplement-related liver injuries. Many people don’t realize these products aren’t tested like drugs. No one checks their purity. No one tracks side effects. And your doctor might not even ask if you’re taking them.
A 2023 survey found that 68% of people who take supplements don’t tell their doctor. One Reddit user wrote: “My naturopath said my liver enzymes were high because I was ‘detoxing.’” That’s not a thing. Your liver doesn’t “detox.” It just gets damaged.
How Doctors Diagnose It - And Why It’s So Hard
There’s no single test for DILI. Blood tests show elevated liver enzymes - ALT, AST, alkaline phosphatase - but those can rise for many reasons: viruses, alcohol, fatty liver. So doctors use something called the RUCAM score. It’s a checklist that looks at:
- When you started the drug
- How long you took it
- Did symptoms improve after stopping?
- Did you take other drugs?
- Are you drinking alcohol?
- Is there another explanation?
It’s not perfect, but it’s the best tool we have. And it only works if you tell your doctor everything you’re taking - even the “natural” ones.
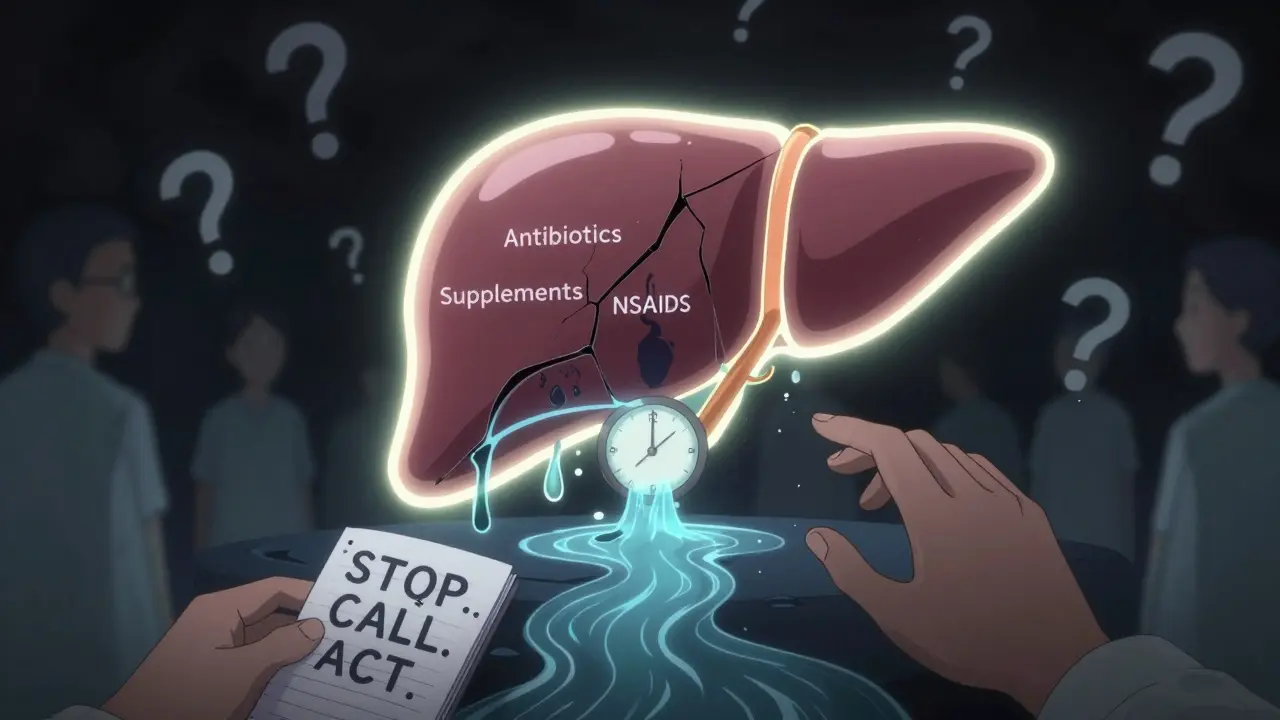
What Happens After Diagnosis?
First thing: stop the drug. Always. Even if you think it’s helping. The liver can heal - if you act fast. Most people recover fully within weeks or months. But some develop chronic liver damage. A few need transplants.
For acetaminophen overdose, N-acetylcysteine is given intravenously. For other drugs, there’s no antidote. Just rest, fluids, and monitoring. Your doctor will check your liver enzymes weekly until they drop back to normal.
High-risk drugs like isoniazid (used for tuberculosis) require regular blood tests. The Cleveland Clinic recommends checking liver enzymes every 4 weeks for people on this drug. Ten percent of users will have abnormal results. Catching it early saves lives.
Prevention Is Simple - But Nobody Does It
You can protect yourself with three simple steps:
- Keep a medication log - write down every pill, capsule, tea, or powder you take. Include brand names, doses, and start dates.
- Never mix alcohol with medications - it multiplies liver damage risk by 3 to 5 times.
- Ask your doctor or pharmacist - “Is this medicine hard on the liver?” before you start it.
And if you’re taking supplements? Check if they’re on the British Liver Trust’s list of high-risk products. Avoid anything that doesn’t list ingredients clearly. No label? No chance.
The Future - And Why You Should Care
New tools are coming. The FDA approved a phone app called DILI-Alert in 2023. It scans your meds and warns you if they’re risky. AI systems are cutting diagnosis time by 35%. But none of this helps if you don’t know the signs.
Right now, 42% of UK GPs still can’t correctly identify the most common hepatotoxic drugs. And 68% of supplement users have no idea they’re at risk. That’s why this matters. Your liver doesn’t scream until it’s too late. But if you know what to look for - and act fast - you can stop it before it breaks.
Can over-the-counter painkillers damage my liver?
Yes, especially acetaminophen (paracetamol). Taking more than 3,000 mg in a day - even spread out - can cause serious liver injury. Many cold and flu remedies contain acetaminophen, so you might be doubling up without realizing it. The risk jumps dramatically if you drink alcohol while taking it.
Are herbal supplements safer than prescription drugs for my liver?
No. In fact, herbal and dietary supplements cause about 20% of all medication-related liver damage in the UK. Products like green tea extract, kava, and high-dose vitamin A have led to liver failure. Unlike prescription drugs, supplements aren’t tested for safety before they’re sold. There’s no monitoring system. And many people don’t tell their doctors they’re taking them.
How long after starting a new medication does liver damage usually appear?
It varies. Antibiotics like amoxicillin-clavulanate often cause damage within 1 to 8 weeks, with an average of 15 days. Anticonvulsants take longer - around 45 days on average. Herbal supplements can show up anytime, from a few days to over a year. Acetaminophen overdose shows signs within 24 hours. If you notice new symptoms after starting a new drug, don’t assume it’s unrelated.
If my liver enzymes are slightly high, should I be worried?
Slightly elevated enzymes (1-2 times above normal) are common and often harmless - caused by things like fatty liver or mild illness. But if they’re more than 3 times above normal, especially with symptoms like fatigue, dark urine, or itching, it’s a red flag. If you’ve started a new medication recently, stop it and see your doctor immediately.
Can I get liver damage from a medication I’ve taken for years?
Yes. While most cases happen within the first few weeks, some people develop liver injury after months or even years of use. This is more common with drugs like statins or anticonvulsants. It’s unpredictable. That’s why it’s important to report any new symptoms - even if you’ve been on the drug for a long time.
What should I do if I think I have medication-related liver damage?
Stop taking the suspected medication immediately. Call your doctor or go to A&E if you have jaundice, dark urine, or abdominal pain. Don’t wait for an appointment. Bring a list of all medications and supplements you’ve taken in the last 3 months. The sooner you act, the better your chances of full recovery.




