If you've spent years with a cigarette in your hand, you know the risks. But here is the reality: lung cancer is often a silent climber, reaching advanced stages before any symptoms actually appear. By the time a cough or chest pain starts, the options for treatment are often limited. This is why low-dose CT is a specialized medical imaging test designed to find lung cancer early when it is most treatable. Also known as an LDCT scan, this tool doesn't just look for problems; it actively reduces the risk of dying from the disease by catching tumors while they are still small enough to be surgically removed.
Who Actually Qualifies for Screening?
Not everyone who has smoked needs a scan every year. To avoid unnecessary radiation and anxiety, medical experts have set specific boundaries. Based on the updated guidelines from the
U.S. Preventive Services Task Force (USPSTF), you generally qualify if you meet these three criteria:
Now, the "pack-year" part usually confuses people. It is a simple math problem: multiply the number of packs you smoke per day by the number of years you've smoked. For example, if you smoked one pack a day for 20 years, that is 20 pack-years. If you smoked two packs a day for 10 years, that is also 20 pack-years. If you've been smoke-free for more than 15 years, the benefit of screening drops significantly, and doctors typically recommend stopping the annual scans.
The Low-Dose CT Process: What to Expect
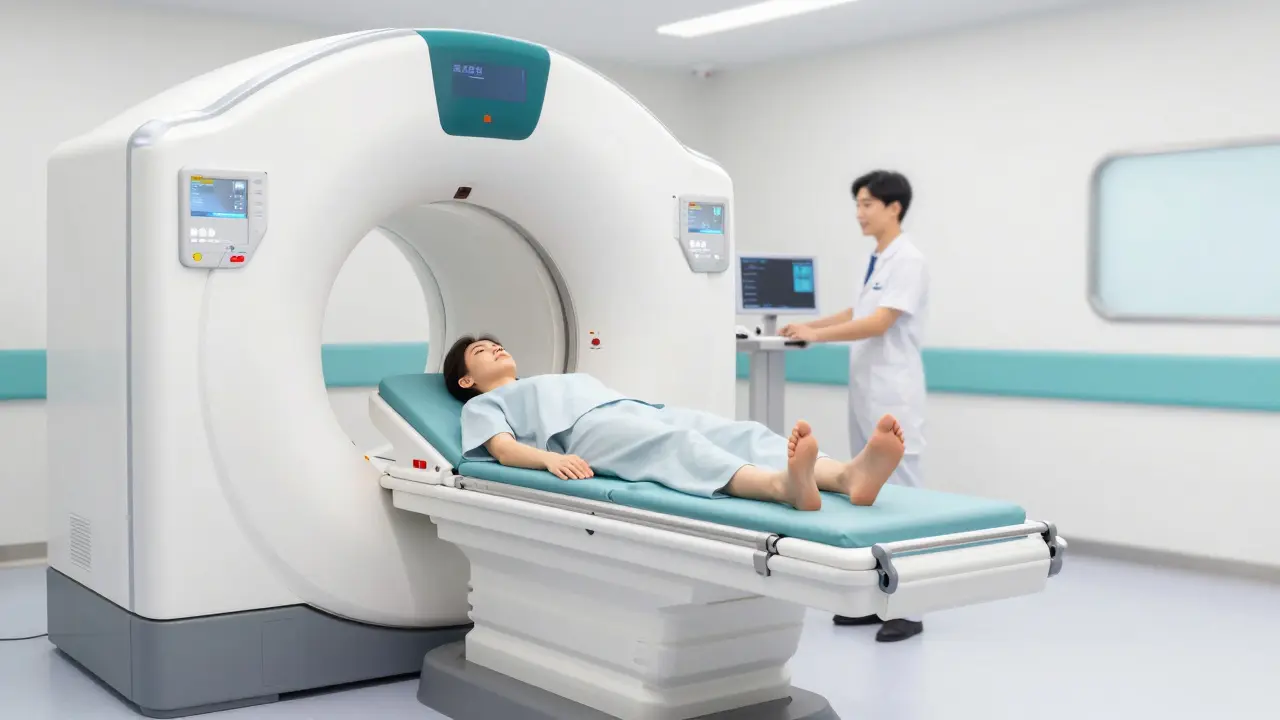
Forget the claustrophobic tunnels of some MRI machines. An LDCT is a non-invasive X-ray procedure that takes detailed cross-sectional images of the lungs using a lower dose of radiation than a standard CT scan.
The process is incredibly fast-usually taking less than 10 minutes. You simply lie on a table while the scanner slides over you. Because it is "low-dose," it uses about 1.5 millisieverts of radiation, which is a fraction of the 7-8 millisieverts used in a diagnostic CT. You don't need any dyes or injections, and there is no recovery time. You can literally walk in, get scanned, and go back to your day.
| Feature | Low-Dose CT (LDCT) | Standard CT Scan |
|---|---|---|
| Radiation Dose | ~1.5 mSv | 7-8 mSv |
| Primary Purpose | Early Screening/Detection | Detailed Diagnosis/Treatment Planning |
| Procedure Time | Under 10 minutes | Varies (often longer) |
| Typical Use Case | High-risk smokers without symptoms | Patients showing active symptoms |
The Trade-off: Benefits vs. False Positives
No medical test is perfect. While the National Lung Screening Trial (NLST) showed a 20% reduction in mortality compared to old-school chest X-rays, there is a catch: false positives.
A false positive happens when the scan finds a small nodule that looks suspicious but turns out to be harmless scar tissue or a benign growth. In the NLST, about 13.9% of screening rounds resulted in false positives. This can lead to a "medical merry-go-round" where you undergo repeated scans or even invasive biopsies for something that was never cancer. For some, this causes significant anxiety and psychological stress. However, the trade-off is generally considered worth it: finding a Stage 1 tumor early can be the difference between a curative surgery and palliative care.
Navigating the Healthcare System
Getting the scan is only half the battle; you need to go to the right place. For a screening to be effective and covered by insurance (like Medicare), the facility should be ACR-accredited is a certification from the American College of Radiology ensuring the facility meets strict quality and safety standards for lung cancer screening.
When you get your results, don't panic if you see a code. Doctors use the Lung-RADS (Lung Imaging Reporting and Data System) to standardize reports. A Category 1 means everything looks normal. A Category 4 means there is something highly suspicious that needs immediate action. Knowing where you fall on this scale helps you and your doctor decide if you need a follow-up in three months or a biopsy right away.
Common Barriers and How to Overcome Them
Surprisingly, many people who qualify never get scanned. Some simply don't know they are eligible, while others fear the results. In some regions, the nearest accredited center might be a long drive away. To get through this, start with a "shared decision-making visit." This is a 20-30 minute conversation with your primary doctor to weigh the risks of radiation and false positives against the benefit of early detection.
If you are struggling to find a provider, ask your clinic if they have a nurse navigator. These specialists help high-risk patients schedule their scans and manage the follow-up appointments, which significantly increases the likelihood that you'll actually complete the annual screening cycle.

What is Next for Lung Screening?
We are moving beyond the simple "pack-year" math. Newer risk models, like the PLCOm2012, are beginning to look at family history, education levels, and respiratory symptoms to better predict who actually needs a scan. We are also seeing the rise of AI. The FDA has already cleared software like LungAssist by VIDA Diagnostics, which helps radiologists spot nodules more accurately and has shown a 15.2% reduction in false positives.
The goal is to move toward "personalized screening"-where the frequency and timing of your scan are tailored to your specific biological risk rather than just how many cigarettes you smoked in the 90s.
Does Medicare cover lung cancer screening?
Yes, Medicare generally covers annual LDCT screenings for adults aged 50-77 who meet the smoking history requirements (20 pack-years and current/recent smoker). You must have a documented shared decision-making visit with your provider before the scan is ordered.
How often should I get a low-dose CT scan?
If you meet the eligibility criteria, the recommendation is for an annual screening. This means one scan every 12 months to monitor for any new or growing nodules.
Is the radiation in an LDCT scan dangerous?
The radiation dose is significantly lower than a standard CT (about 1.5 mSv). While any radiation carries a small risk, the medical consensus is that the potential to save a life through early cancer detection far outweighs the risk of the low-dose radiation.
What happens if the scan finds a "nodule"?
Finding a nodule is common and does not always mean you have cancer. Depending on the Lung-RADS score, your doctor may suggest "watchful waiting" with another scan in a few months to see if the nodule grows, or they may order a biopsy if the nodule looks suspicious.
When should I stop getting screened?
You should typically stop annual screening if you have not smoked for 15 consecutive years, or if you develop a health condition that severely limits your life expectancy or your ability to undergo curative lung surgery.
Next Steps for Patients
If you fit the 50-80 age bracket and have a 20 pack-year history, your next move is to schedule a consultation with your primary care provider. Don't just ask for a scan; ask for a "shared decision-making visit." During this time, discuss your specific risk factors, including any family history of lung cancer.
If you are a former smoker who quit more than 15 years ago, you might not qualify for the annual program, but you should still mention any lingering respiratory symptoms to your doctor. For those who qualify, ensure the facility you choose is ACR-accredited to ensure you get the most accurate results and the best follow-up care.





Comments (2)