| Feature | Allergic Asthma (Overlap) | Non-Allergic Asthma |
|---|---|---|
| Typical Onset | Usually childhood (70% before age 12) | Often develops in adulthood |
| Main Triggers | Pollen, dust mites, pet dander, mold | Stress, exercise, cold air, pollutants |
| ICS Response | High (60-70% achieve good control) | Moderate (40-50% achieve good control) |
| Symptom Pattern | Strongly seasonal or trigger-dependent | More consistent or environment-neutral |
The Science Behind the Squeeze
To fix the inflammation, you have to understand what's actually happening in your lungs. In a typical asthma-allergy overlap, your immune system overreacts to a harmless substance, like a speck of dust. This triggers the production of IgE is an antibody produced by the immune system that binds to mast cells and triggers the release of histamine during allergic reactions. Once these antibodies are activated, they tell your mast cells to dump chemicals that make your airways swell and produce excess mucus. This creates a complex inflammatory pattern involving eosinophils-white blood cells that can cause significant tissue damage if left unchecked. According to the Global Initiative for Asthma (GINA), the leading international organization that provides evidence-based guidelines for the management of asthma, this often follows the "allergic march." This is a progression where a child starts with eczema, moves to allergic rhinitis (hay fever), and finally develops asthma. If you have any two of these, the third is often just around the corner.Breaking the Cycle: How to Identify Your Triggers
You can't fight an enemy you can't see. Many people spend years simply treating the symptoms with a rescue inhaler without ever knowing why the attack started. The gold standard for identifying these culprits is Skin Prick Testing is a diagnostic procedure where small amounts of common allergens are introduced into the skin to observe the immune response. It has about a 95% sensitivity rate for common aeroallergens, making it the most reliable way to map your triggers. Beyond skin tests, doctors look for elevated specific IgE levels in your blood. When these results are paired with Spirometry is a pulmonary function test that measures the quantity and speed of air an individual can inhale and exhale, a clear picture emerges. If your airflow obstruction is reversible and you have a positive allergy test, you're dealing with the overlap. Identifying these triggers is the single most important step toward long-term control; without it, you're essentially playing a game of whack-a-mole with your symptoms.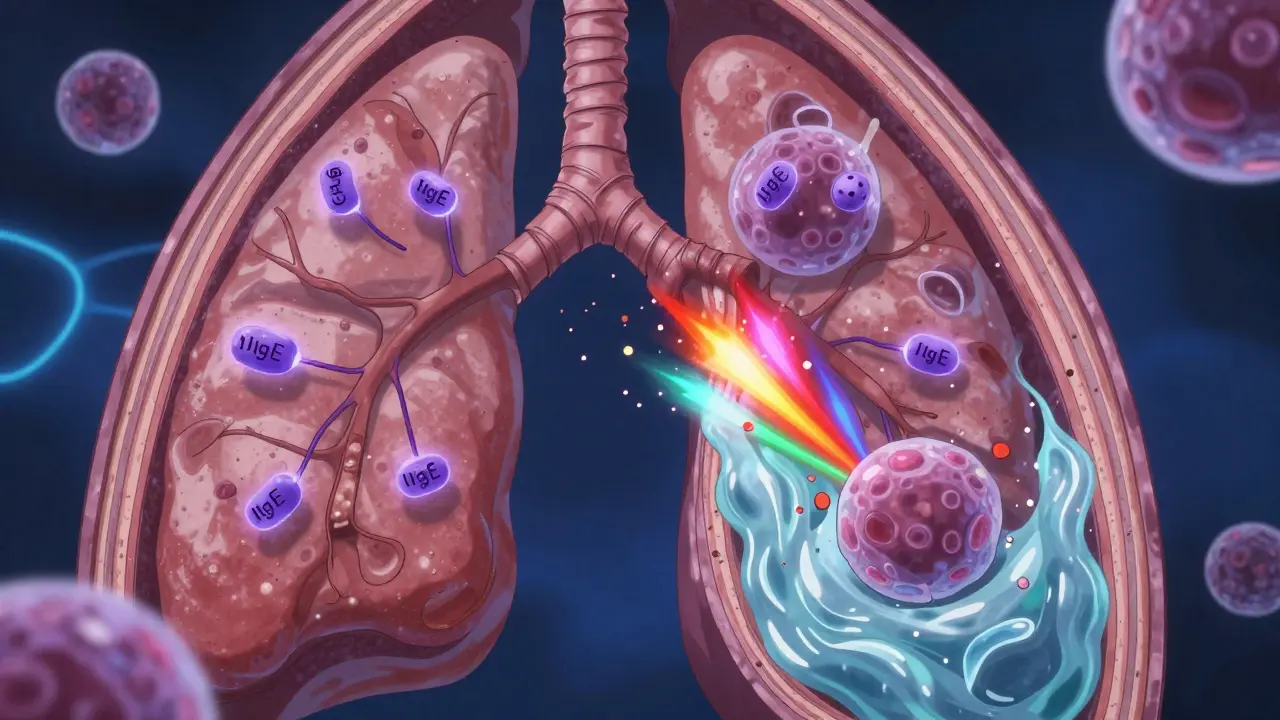
Practical Strategies for Airway Control
Once you know what's triggering the inflammation, the goal is to lower the "allergic load" on your system. This isn't about living in a bubble, but about making smart, concrete changes to your environment.- The Dust Mite Defense: Use allergen-proof bedding. While it sounds simple, only about 55% of people stick with this long-term. Switching to a vacuum with a HEPA filter can reduce dust mite allergens by 85% if used weekly.
- Hyperlocal Tracking: General weather reports aren't enough. Using apps like Allergy Alert allows you to see real-time pollen counts in your specific neighborhood, helping you decide if today is a "stay indoors" day.
- The Pet Compromise: If you're allergic to cat or dog dander, you don't always have to rehome your pet. However, keeping the bedroom a pet-free zone can drastically reduce the amount of rescue inhaler use-one patient reported dropping from four uses a week to once a month just by doing this.
Advanced Treatments: Immunotherapy and Biologics
When avoiding triggers and using inhalers isn't enough, it's time to look at disease-modifying treatments. Unlike steroids, which just manage the inflammation, Allergen Immunotherapy is a treatment that involves exposing the patient to increasing doses of an allergen to desensitize the immune system actually trains your body to stop overreacting. Immunotherapy can lead to a 40-60% reduction in asthma symptoms. However, it requires patience. The initial "build-up" phase can last 3-6 months and is often the hardest part, with some patients experiencing temporary symptom spikes. The long-term payoff is huge: a 3-5 year commitment can reduce long-term medication costs by roughly $1,200 annually. For those with severe allergic asthma that doesn't respond to standard care, Biologic Therapies are highly targeted medications, such as monoclonal antibodies, that block specific molecules in the inflammatory pathway the new frontier. For example, Omalizumab (anti-IgE) can reduce exacerbations by 50%. More recently, the FDA approved Tezepelumab, which works for both allergic and non-allergic severe asthma, showing a 56% reduction in attacks regardless of the patient's eosinophil count. While biologics are expensive-often costing $25,000 to $35,000 a year-they provide a lifeline for those who would otherwise be frequently hospitalized.Navigating the Challenges of Long-Term Care
Managing this overlap is a marathon, not a sprint. One of the biggest hurdles is the "treatment gap." Many primary care physicians only screen about 35% of their asthma patients for allergies, whereas board-certified allergists do it 65% of the time. If your current doctor hasn't sent you for allergy testing, it's time to ask for a referral. There's also the frustration of insurance and cost. Comprehensive testing can cost between $250 and $400 out-of-pocket for some. Furthermore, the time commitment for weekly allergy shots is a common reason why about 31% of patients drop out of immunotherapy within the first year. To succeed, you need a system: mark your shots on a digital calendar, use a HEPA filter on a recurring weekly reminder, and keep a symptom diary to track how your airway inflammation responds to new treatments.Can I outgrow asthma-allergy overlap?
While some children may see a reduction in allergic symptoms as they grow, the underlying tendency toward airway inflammation often persists. However, allergen immunotherapy can effectively "desensitize" the system, meaning that while the asthma isn't necessarily "cured," the triggers no longer cause severe reactions.
How do I know if my asthma is allergic or non-allergic?
The best way is through clinical testing. Allergic asthma typically presents with seasonal spikes, a history of childhood eczema or hay fever, and positive results on a skin prick test or specific IgE blood test. Non-allergic asthma is often triggered by non-immune factors like cold air or exercise and doesn't show these allergic markers.
Are allergy shots safe for everyone with asthma?
Most patients tolerate immunotherapy well, but it must be administered under medical supervision because of the risk of systemic reactions. Patients with severe, uncontrolled asthma may need to stabilize their airway inflammation with corticosteroids before starting immunotherapy to ensure safety.
Which is better: immunotherapy or biologics?
It depends on the severity. Immunotherapy is more cost-effective and aims for long-term desensitization, but it takes years to reach full effect. Biologics are designed for severe, refractory asthma and work much faster to block inflammation, but they are significantly more expensive and usually require ongoing administration.
Does a HEPA filter actually help with asthma?
Yes, specifically for those with the asthma-allergy overlap. HEPA filters are designed to trap tiny particles, including dust mite allergens and pollen. Using a certified HEPA vacuum weekly has been shown to reduce dust mite allergens by up to 85%, which directly lowers the trigger load on your airways.