Understanding the Link Between Skin and Joints
To get why this happens, we have to look at the immune system. In a healthy body, your immune system fights off viruses and bacteria. But with an autoimmune disease, the system gets confused and starts attacking healthy tissues. Specifically, the body produces proteins that trigger inflammation in the skin and the areas where tendons attach to bone. Psoriasis is a chronic skin condition characterized by red, scaly patches covered with silvery scales, known as plaques. When this inflammation spreads to the joints, it becomes psoriatic arthritis (PsA). This isn't just "stiff joints"; it's a progressive disease. If left untreated, it can lead to permanent bone erosion and joint deformity. Experts have found that certain genetic markers, like the HLA-B27 allele, can make someone more prone to this specific type of inflammatory response.Spotting the Warning Signs
PsA doesn't look the same for everyone. Some people feel it in their lower back, while others notice it in their fingertips. There are a few "red flag" symptoms that are very specific to this condition:- Dactylitis: This is often called "sausage digits." Instead of just one joint hurting, the entire finger or toe swells up, making it look like a small sausage. This happens in about 40% of patients.
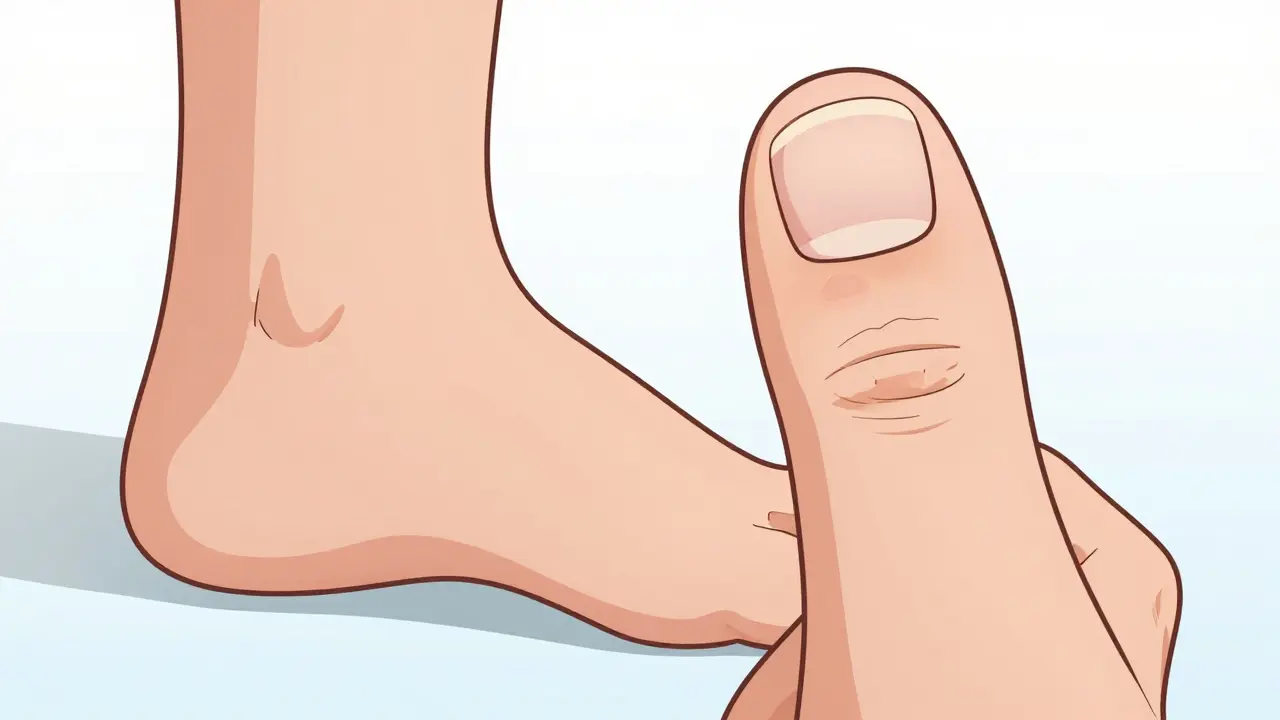
- Enthesitis: This is inflammation where a tendon or ligament connects to the bone. A classic example is pain in the Achilles tendon or the sole of the foot.
- Nail Changes: Keep an eye on your nails. Pitting (tiny dents), thickening, or the nail lifting away from the bed happens in about 80% of PsA patients and is a huge clue for doctors.
- Plaque Psoriasis: Those red, scaly patches are present in the vast majority of cases, typically covering varying percentages of the body.
How Doctors Actually Diagnose PsA
Because PsA can mimic rheumatoid arthritis or osteoarthritis, doctors use a specific scoring system called the CASPAR criteria is a clinical classification system designed to identify psoriatic arthritis by weighing skin, nail, and joint symptoms. To get a diagnosis, a doctor doesn't just look at one thing. They use a combination of your medical history, physical exams, and tests. They might check your blood for inflammatory markers like C-reactive protein (CRP) or the erythrocyte sedimentation rate (ESR). If they see bone erosion on an X-ray-sometimes appearing as a "pencil-in-cup" deformity where the bone narrows and then widens-it's a strong indicator of established disease.| Criterion | Points |
|---|---|
| Current Psoriasis (Skin/Scalp/Nails) | 2 Points |
| Personal History of Psoriasis | 1 Point |
| Family History of Psoriasis | 1 Point |
| Nail Dystrophy (Pitting/Onycholysis) | 1 Point |
| Negative Rheumatoid Factor (RF) | 1 Point |
| Radiographic Evidence of Joint Damage | 1 Point |
Note: A total score of 3 or more is generally required to confirm a diagnosis of PsA.
Treatment Strategies: From Pills to Biologics
Treating PsA is about more than just stopping the pain; it's about preventing the joints from fusing or eroding. Doctors usually follow a stepwise approach, starting with the gentlest options and moving up as needed.- NSAIDs: For mild symptoms, nonsteroidal anti-inflammatory drugs help reduce swelling and pain.
- DMARDs: When the disease persists, doctors use Disease-Modifying Antirheumatic Drugs is a class of medications, such as methotrexate, that slow down the progression of joint damage by suppressing the overactive immune system. Methotrexate is a common first choice here.
- Biologics: For moderate to severe cases, Biologic Therapy is advanced medication engineered from living organisms to target specific parts of the immune system, such as TNF inhibitors or IL-17 inhibitors. These are game-changers. They target specific proteins like Tumor Necrosis Factor alpha (TNF-α). If you have severe skin plaques, an IL-17 inhibitor might be the better choice, whereas TNF inhibitors are often preferred for spinal involvement.
- JAK Inhibitors: If biologics don't work, newer oral medications called JAK inhibitors can block the signaling pathways inside cells to stop inflammation.
The Hidden Dangers: Comorbidities
Here is something most people don't realize: PsA isn't just about skin and joints. Because it's a systemic inflammatory disease, the inflammation doesn't always stay in one place. It can affect your heart and your mood. About 40-50% of people with PsA also deal with cardiovascular disease. The chronic inflammation in the body can damage the lining of the blood vessels, leading to a significantly higher risk of heart attacks compared to the general population. Metabolic syndrome-a mix of high blood pressure, high blood sugar, and excess belly fat-is also incredibly common. Then there's the mental toll. Dealing with chronic pain and visible skin lesions is exhausting. Between 20% and 30% of patients struggle with depression and anxiety. This creates a vicious cycle: stress can trigger a psoriasis flare, and the flare can lead to more stress and joint pain.
The Future of Precision Medicine
We are moving away from a "one size fits all" approach. In the coming years, doctors will likely use biomarkers-specific proteins in your blood-to predict which medication will work for you before you even take the first dose. Researchers are also looking into the "gut-skin-joint axis," discovering that the bacteria in your gut might play a role in how your immune system reacts. Newer drugs targeting IL-23 and TYK2 are showing promise in clinical trials. The goal is to reach "Minimal Disease Activity," which means almost no swollen joints, minimal skin involvement, and a return to normal daily functioning. Early intervention is key; the sooner you start the right therapy, the better your chance of avoiding permanent disability.Can psoriasis be cured?
Currently, there is no permanent cure for psoriasis or psoriatic arthritis because they are chronic autoimmune conditions. However, they can be managed so effectively with modern biologics and lifestyle changes that many people achieve complete remission, where their skin is clear and their joints pain-free.
Does psoriatic arthritis always follow psoriasis?
Not always. While about 85% of people develop skin plaques first, around 5-10% of people experience joint inflammation before any skin symptoms appear. This is why joint pain in people with a family history of psoriasis should be taken seriously.
What is the difference between RA and PsA?
Rheumatoid arthritis (RA) typically affects smaller joints symmetrically and is often associated with rheumatoid factor in the blood. Psoriatic arthritis (PsA) involves skin and nail changes, dactylitis (sausage toes), and is usually "seronegative," meaning the rheumatoid factor is absent.
Are there any dietary triggers for PsA?
While no specific diet cures PsA, inflammation is often worsened by processed sugars and saturated fats. Many patients find that an anti-inflammatory diet (like the Mediterranean diet) helps manage symptoms, and emerging research into the gut microbiome suggests that gut health is closely linked to joint inflammation.
How do I know if my joint pain is PsA or just aging?
Standard "wear and tear" arthritis usually feels worse after activity. PsA inflammatory pain often feels worst in the morning (morning stiffness) and may actually improve with movement. If you have a history of skin issues or notice swelling in the entire digit, see a rheumatologist.




